 Simulation and Procedure Labs
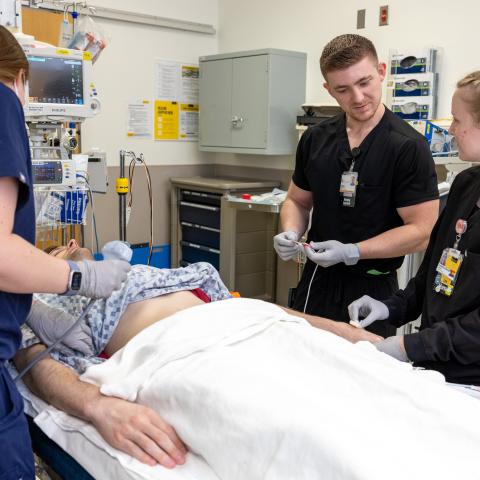
Simulation and Procedure Labs
Simulation is an evolving area of medical education and plays an integral role in healthcare training. With Emergency Medicine’s broad spectrum of pathologies and presentations encountered, the requirement for proficiency in numerous procedural skills, and the importance of high-stakes communication simulation plays an important role in an EM curriculum.
The University of Iowa has dedicated faculty with special expertise and focus on simulation education (Certified Healthcare Simulation Educators). The residency program partners with the Center for Procedural Skills and Simulation to utilize a full range of infant, pediatric and adult manikins and procedural task trainers to meet our diverse educational needs. Case content is continually revised to reflect the most up-to-date medicine and offers learners the opportunity to encounter a broad variety of high stakes clinical scenarios in a learning environment that fosters growth for all learners.
Throughout your residency, you will have many opportunities to learn and reinforce concepts in effective patient care, procedures, communication and teamwork through simulation. Faculty develop new and engaging simulation cases and procedure workshops on an ongoing basis to meet the evolving needs of EM. Residents participate in a monthly simulation and procedure lab as well as annual sessions to help prepare you for ABEM’s certification examination. Emergency department in situ simulations occur quarterly and residents have the opportunity to participate while working clinical shifts. Residents participate in an annual rare procedures day with guidance from emergency medicine and other specialty service faculty that cover skills such as thoracotomy, surgical airways, chest tube placement, central line placement and other vascular access techniques, transvenous pacemaker placement, umbilical line placement, gastric tube placement, advanced orthopaedic skills, lateral canthotomy and cantholysis, advanced facial laceration repair, and nerve blocks. Emergency medicine faculty coordinate, act and judge for a lively and fun annual simulation-based competition. All simulations utilize structured debriefing methods to assure learners get the maximal benefit from the experiences.
Learners with special interest in simulation are welcomed and encouraged to work with our simulation faculty on case development or educational research to help prepare them to pursue a career in simulation-based education after residency. Residents have successfully developed and conducted simulations for academic or research related projects including receiving grant funds to support these projects.