About the Program
Welcome to the University of Iowa Pulmonary and Critical Care Fellowship Training Program website.
What makes Iowa an extraordinary place to advance your career? It starts with our commitment to your training. At Iowa you become proficient in clinical care while exploring for new knowledge to take that care to the next level. Simply put, our fellowship training program is our highest priority and we are blessed with a faculty who love to teach and learn in an academic environment. To learn more about our training program, contact us today. We want to tell you more about Iowa!
Mission Statement
We strive to deliver compassionate state-of-the-art care for patients, educate the next generation of physicians and scientists, and discover new ways to cure disease and prevent illness.
Vision
Through delivery of patient care, education and discovery, we will work to prevent and treat respiratory, environmental, and work-related diseases and critical illnesses. We will accomplish this in a multidisciplinary, safe and supportive work environment, always respectful of the public trust.
Goals
- Provide high-quality and compassionate health care for patients with respiratory, environmental and work-related diseases and critical illnesses at the University of Iowa Hospitals and Clinics, the Iowa City Veterans Affairs Medical Center, and their affiliated community programs.
- Provide outstanding educational programs for all learners in the health professions and in the biomedical sciences to ensure acquisition of knowledge and skills commensurate with the needs of society
- Develop new knowledge about human biology by conducting a spectrum of important research related to the pathogenesis, prevention, diagnosis and treatment of human disease.
- Provide a work environment that engenders mutual respect, facilitates satisfaction, and fosters career development for all who carry out or participate in our missions.
- Demonstrate through our actions the highest standards of professional and ethical behavior.
- Provide regional, national and international leadership for the betterment of society.
Clinical Training: Year 1
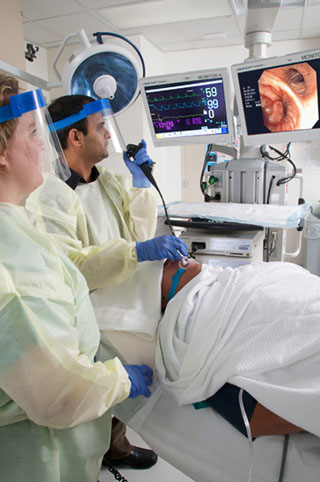
The first year of the fellowship is primarily a clinical year of training in both Pulmonary and Critical Care Medicine, care of inpatients and outpatients, and development of proficiency in various procedures including endotracheal intubation, chest tube insertion, bronchoscopy, thoracentesis, and interpretation of pulmonary function tests. Each fellow spends 6 months in the first year working in the University medical intensive care unit. During 3 of these months they also rotate through the pulmonary procedures laboratory ~3 afternoons per week performing bronchoscopy and ultrasound guided thoracentesis. 3 months are spent at the VA hospital - across the street from University of Iowa Hospitals & Clinics. One month each is spent on the anesthesia, surgical ICU and thoracic surgery services.
Medical Intensive Care Unit (UI Hospitals & Clinics)
The MICU is a 26-bed closed unit which averages >200 admissions per month. Two fellows are assigned to the MICU each month. They work closely with the attending physician and provide clinical oversight of the 6 house officers and senior medical students on the service. The fellows are responsible for performing and/or supervising all invasive procedures including endotracheal intubation, bronchoscopy, chest tube insertion, central line placement, etc. The pulmonary/critical division provides airway management services for the majority of our MICU patients – each fellow performs on average ~100 intubations during the first year of training.
Procedures (UI Hospitals & Clinics)
During three of the six MICU months the fellow spends ~3 afternoons per week working in the procedures laboratory performing bronchoscopy, thoracentesis and chest tube thoracostomy. This is a state-of-the-art facility which opened in 2000. Fellows are trained in endobronchial ultrasound (EBUS) and participate in a variety of interventional bronchoscopy procedures. The average number of bronchoscopies performed during the F1 year is ~75 with over 200 done during the three years of fellowship training.
VA Hospital
Each fellow spends 3 months at the VA hospital during their 1st year. Responsibilities include working with the attending physician supervising the care of patients in the medical intensive care unit, providing subspecialty consultation, performing procedures, interpreting pulmonary function tests and seeing patients in the clinic.
Lung Transplant/Thoracic Surgery
During the month the fellows are actively involved in the inpatient and outpatient evaluation of lung transplant candidates and recipients.
They have the opportunity to observe a variety of surgeries including lung resection, decortication of empyema, lung transplantation, and mediastinoscopy. They gain a thoracic surgical perspective on the placement and management of chest tubes.
Anesthesia
During this 1 month rotation fellows work in the operating room setting improving their airway management skills through training with our anesthesia colleagues. This includes assessment of airway difficulty, pre-oxygenation techniques, bag-mask ventilation, rapid sequence intubation, LMA placement, use of double lumen endotracheal tubes and other skills.
Surgical ICU
Each fellow spends 1 month in the surgical ICU working with a variety of patients from all the surgical services including orthopedic, trauma, neuro, cardiothoracic, vascular, urology, gynecology and general surgery. Each fellow oversees a 10-bed bay, working closely with a surgical critical care attending physician. During this month they gain a unique surgical perspective in the treatment of critical illness.
Vacation
Each fellow receives 4 weeks of vacation/personal time per year. In the 1st year vacation is taken during the SNICU, TCV and anesthesia rotations.
Clinical Training: Years 2 and 3
Pulmonary Consultation Service (UI Hospitals & Clinics inpatient)
During their second and third year of training fellows spend 1.5 months/year on the inpatient pulmonary consultation service. They see an extremely wide array of pulmonary and critical care diseases and learn the art of functioning as a subspecialist consultant.
Procedures/Physiology Service
During their second and third years of training fellows spend 1.5 months/year on a multidisciplinary service where they perform pulmonary procedures in the morning (bronchoscopy, thoracentesis, etc) and attend sleep medicine and pulmonary rehabilitation clinics and perform cardiopulmonary exercise tests in the afternoon.
Subspecialty Clinics
Each fellow attends subspecialty clinics ½ day/week for a total of six months during their second and third year. A wide variety of subspecialty clinic experiences are available including lung cancer, cystic fibrosis, TB, interstitial lung disease, asthma, occupational medicine, sleep medicine, lung transplantation and pulmonary hypertension.
Continuity of Care (COC) Clinic
Each fellow has a COC clinic throughout their three years of fellowship. During the 1st year fellows have clinic for a total of 8 months. During all of the second and third years fellows have clinic ½ day each week – rotating between UI Hospitals & Clinics and VA Medical Center. These clinics are staffed by attending physicians dedicated to the fellow’s clinic - chosen specifically for their teaching interest and ability. The clinic patient mix encompasses the entire spectrum of pulmonary medicine.
Career Pathways
The training goal of our division is to provide mentorship and guidance for each fellow to develop a career path that best fits his or her interests and aspirations. The University of Iowa Pulmonary/Critical Care Division has developed four career paths: Master Clinician Pathway; Medical Education Pathway; Clinical Investigator Pathway and Basic Research Pathway. The different career paths are designed to produce physicians who will have the skills and training to become leaders in their field of expertise - in academic medicine or in the community. The common threads throughout each path are the pursuit of excellence and contribution to scholarship (broadly defined). Fellows will identify a career path at the end of their first year and then work with their individual mentors and the program leadership to develop an individualized comprehensive curriculum. It is important to recognize that these pathways are not “silos” – there may be crossover or hybridization between them – depending on the goals and aspirations of each fellow.
Master Clinician Pathway
The goal of the Master Clinician Pathway is to develop the skills and knowledge to provide specialized patient care at the highest level – and to be a “go to” clinical leader at the national and/or local level. Master Clinicians should also be educators and may also participate in clinical research. Requirements (final requirements determined by each fellow’s mentoring committee) for this pathway include:
- Completion of common core requirements
- Two (or more) additional months of clinical service in both the second and third year of fellowship. This would usually involve more general training in the second year and more specialized training in the third year. The potential clinical services are diverse and include – ICU training in the SICU, CVICU or Burn Unit, RSCU, Anesthesia, consultative services both within and outside the Division/Department, Sleep Medicine Training, echocardiography, right heart catheterization, etc.
- Chest Radiology Training.
- Completion of the FACE program.
- Additional subspecialty clinic experience – as determined by the specific interests of the fellow.
- Completion of the University of Iowa Department of Internal Medicine Quality Improvement and Patient Safety Fellows curriculum – with development and completion of a Patient Safety/QI project.
- Scholarly Activity: examples - completion of a book chapter, review article, case report or manuscript of a QI/PS project.
- Involvement in case conferences, lectures, etc - as determined by the specific interests of the fellow.
- Attendance at a national meeting - ATS, ACCP, etc – in each of the second and third years.
- Mentoring committee review meetings every six months during the second and third years.
Medical Education Pathway
The goal of the Medical Education Pathway is to prepare the fellow for an academic career in medical education. This pathway also recognizes that clinical expertise plays a foundational role in clinical education. Requirements (final requirements determined by each fellow’s mentoring committee) for this pathway include:
- Completion of common core requirements.
- Completion of the Masters or Certificate Program in Medical Education (tuition supported by the division)
- Completion of a Patient Safety/Quality Improvement project – potentially centered on education.
- Participation in medical student, resident and peer education
- Scholarly activity:
- Development of an educational portfolio with a series of presentations to a diversity of audiences (lay persons, medical students, residents, peer) on an area of clinical interest – with a minimum of 8 self-authored presentations
- Development of a new curriculum project – for example, educational modules for students and/or residents on the pulmonary consultation service.
- Dissemination of research/curriculum development is highly recommended: e.g. publication in a peer-reviewed medical education journal (Journal of Graduate Medical Education for example) or presentation at an education meeting (AAMC for example).
- Attendance at a meeting focused on medical education – PCCM Program Director Meeting, AAMC or ACGME regional/national meetings.
- Mentoring committee review meetings every six months during the second and third years.
Clinical Research Pathway
The goal of the Clinical Research pathway is to develop the skills and expertise for a successful academic career in Clinical Research.
- Completion of common core requirements
- Completion of a Master’s degree, Certificate Program or selected coursework in Clinical and Translational Science, Public Health or other graduate program (tuition supported by the division).
- Identification of a research project/mentor(s) – 18 months of clinical research during second and third years of fellowship (minus time devoted to COC and subspecialty clinics and sleep medicine/exercise testing requirements).
- Scholarly activity:
- Development of a research proposal – with submission to the IRB if appropriate
- Presentation/publication of research
- Apply for peer-reviewed funding – if appropriate, depending on the research project.
- Attend a workshop on scientific writing and presentation
- Attendance at 1 (or more) IRB meetings
- Presentation of research yearly at the divisional Research Conference
- Mentoring committee review meetings every six months during the second and third years.
- Option for a 4th and 5th year of research experience supported by the training grant.
Basic Science Research Pathway
The goal of the Basic Science Research pathway is to develop the skills and expertise for a successful academic career in Basic Science Research
- Completion of common core requirements.
- Identification of a research project/mentor(s) – 18 months of basic research during second and third years of fellowship (minus time devoted to COC and subspecialty clinics and sleep medicine/exercise testing requirements).
- Development of a research proposal – with submission to the IRB and/or Animal Care Committee if appropriate
- Presentation (nationally)/publication of research findings
- Apply for peer-reviewed funding
- Attend a workshop(s) on scientific/grant writing and presentation.
- Option for a 4th and 5th year of research experience supported by the training grant.
- Presentation of research yearly at the divisional Research Conference
- Mentoring committee review meetings every six months during the second and third years.
Research Training

A primary goal of the division is to train future academic leaders in the field of Pulmonary and Critical Care Medicine. A large number of research training opportunities exist – both in basic and clinical investigation. During the first year of training fellows identify a research area and mentor. This process is facilitated by faculty Research Conference presentations, the Introduction to Research Conference series and individual meetings with research faculty. The fellow and mentor work together to develop a research project.
Frequently, other investigators, both within and outside the division, contribute their expertise to this process. A high level of interdepartmental collegiality and collaboration at Iowa enhances our fellow’s research training. At the beginning of the second year fellows present their research proposal to the division for constructive feedback. During the second and third years of training fellows have ~18 months of protected time to pursue their research experience. They receive training in hypothesis generation, experimental design and techniques, data interpretation and statistics, and preparation of oral presentations and written manuscripts. They regularly present their work at laboratory meetings. Attendance at regional and national meetings is encouraged and financially supported by the division. For those wanting to pursue a career in research a 4th year of fellowship training is available which is dedicated to research. Fellows also have the opportunity to pursue a Masters Degree in Translational Medicine.
Educational Conferences
The division takes special pride in the quality of our educational conferences. Conference attendance is facilitated by the close proximity of the VA and University hospital, and by the high divisional priority placed on fellow’s formal educational experience.
Conferences include:
-
Clinical Pulmonary/Critical Care Conference
-
Journal Club
-
Core Conference Series:
-
Core Lecture Topics – a three-year series of presentations covering all major content areas of pulmonary and critical care medicine. Experts from outside the division frequently come to share their expertise with us
-
Physiology Conference – a monthly discussion of applied physiology topics
-
Chest Radiology Conference – a bimonthly review of interesting and instructional chest filmsResearch Conference
-
-
Pathology Conference
-
Summer Introductory Lecture Series
-
Multidisciplinary Lung Cancer Conference
-
Introduction to Research Conference
Program Facilities Tour
Learn about our facilities!
Interdisciplinary Fellowship Conference
Below is an example of the Department of Internal Medicine Common Curriculum Schedule. It is shared between Fellows from all divisions of the Department.
Fellows as Clinician Educators (FACE)
The Fellows as Clinician Educators (FACE) Program is designed to introduce future clinician-educators to a set of skills which may be of use in their career. The program presents concepts of educational design and research, lecture development, evaluation, observation and feedback. At the conclusion of the program, FACE participants are required to develop a teaching portfolio.
