Anesthesiology Critical Care Medicine Fellowship
About the Program
Welcome and thank you for your interest in our Critical Care Medicine (Anethesiology) Fellowship.
Our fellowship is a one-year, ACGME-accredited program that is based in the Surgical and Neurosciences Intensive Care Unit (SNICU) and the Cardiovascular Intensive Care Unit (CVICU) at the University of Iowa Hospitals & Clinics.
Our units boast state-of-the-art technology and support services, with a special emphasis on diagnostic and procedural ultrasound. Four ACCM fellows are accepted each year from ACGME-accredited programs in Anesthesia, Surgery, multiple surgical sub-specialties, and Emergency Medicine*. Training at the only tertiary-care academic institution in Iowa, fellows in our program receive broad and comprehensive exposure to all aspects of both surgical and medical critical care medicine. These experiences prepare our fellows to enter the practice of critical care medicine and succeed in any career path they may choose.
Fellows spend nine months in core SNICU/CVICU rotations. These rotations emphasize an evidence-based, multidisciplinary, team-based approach to critically ill patients. The critical care team is intimately involved with the care of all patients in the ICU and high-level support is provided by a team of nutritionists, pharmacists, respiratory therapists, physical therapists and an excellent nursing staff. As they progress in knowledge and skills, fellows are encouraged to take leadership roles in the Unit including leading rounds and making patient-care decisions, educating residents and medical students, becoming involved in ICU management, and championing quality improvement initiatives.
In addition to the nine core ICU months, fellows are allowed three months of elective time and are free to choose among a diverse collection of rotations including echocardiography and bronchoscopy, infectious disease, nephrology, neurology, and research.
The units have their own dedicated echocardiography/ultrasound equipment and fellows are encouraged to learn the use of ultrasound for hemodynamic evaluation and bedside procedures such as thoracentesis and invasive monitor placement. Additionally, the units have dedicated bronchoscopy equipment for the performance of diagnostic and therapeutic bronchoscopies.
In addition to the rich clinical experience, our program maintains a strong didactic program with lecture topics guided by ACGME requirements and fellow interest as well as monthly journal clubs, morbidity and mortality conferences, and guideline reviews.
Fellows are required to complete an academic project during their fellowship. Project examples include, but are not limited to, novel research projects or case reports, involvement in ongoing faculty research projects, quality improvement initiatives, or development of educational modules.
Please take this opportunity to explore the possibilities you will find at the University of Iowa by visiting our departmental website as well as this website for specific curriculum and information about our critical care fellowship program.

Archit Sharma, MBBS, MBA
Program Director, Anesthesia Critical Care Medicine Fellowship
*Per ABA and ABEM policy, Emergency Medicine fellows are required to complete a two-year fellowship, which is offered through our program.
University of Iowa Graduate Medical Education (GME) policies are located here.
Curriculum
All fellow educational activities (lectures, journal clubs, M&M conference, guideline reviews) occur from 10:00-11:00 AM on weekdays (Monday-Friday), unless otherwise noted.
Didactic Lecture Series
Fellows attend fellow-specific didactic lectures several times a week throughout the year. These lectures are presented by faculty from within the intensive care division as well as experts from other departments in the institution. The topics covered during this series provide a comprehensive knowledge of critical care medicine and are selected based on ACGME-published guidelines as well as fellow feedback.
Point of Care Ultrasound and Critical Care Echocardiography
Basic transthoracic cardiac and pulmonary ultrasonography is rapidly becoming a standard of care for intensivitists, because it allows for rapid noninvasive assessment of pulmonary status, hemodynamics, cardiac function, and volume status.
/About_the_Program/IMG_9371_website.jpg)
Critical care fellows at Iowa will have access to a state-of-the-art, high-fidelity transthoracic and transesophageal echocardiography (TTE/TEE) simulator as part of their training. The formal critical care echocardiography curriculum at Iowa includes supervised and independent sessions on the TTE/TEE simulator, supervised exams of volunteer model patients, formal instruction on the use of ultrasound equipment currently available for bedside use in our ICUs, didactic lectures, directed readings, informal bedside teaching from faculty in the course of routine patient care, and an expectation that fellows dedicate significant independent time to ultrasonography study. Fellows will be routinely tested on their knowledge of terminology, anatomy, and recognition of pathology, and will be expected to demonstrate proficiency of transducer manipulation and image acquisition on the TTE/TEE simulator.
An additional elective rotation in clinical echocardiography, that can include hands-on exposure to intra-operative and medical in- or out-patient transesophageal echocardiography as well as proctored interpretation of echocardiographic studies, is available.
By the end of their fellowship, trainees will be expected to able to:
- Recognize the basic physical principles of Ultrasound image formation and imaging planes;
- Define terminology involved in probe and transducer manipulation and orientation;
- Identify common steps required to improve poor image quality;
- Consistently obtain high-quality standard echocardiograpy views on patients; and save and interpret still- and cine-images from these views;
- Identify normal and abnormal cardiac, thoracic, abdominal, and vascular anatomy;
- And apply all these skills to use focused ultrasonography for monitoring patients (for example, to assess intravascular volume status and volume responsiveness) and for diagnosing emergent conditions (such as pneumothorax, significant pulmonary edema, pulmonary embolus or other cause of acute right heart failure, pericardial effusion, a significant decrease in left ventricular function, deep venous thrombosis, and certain intra-abdominal pathology).
Journal Clubs
Journal clubs are held once a month and are attended by fellows and faculty. During each journal club, three fellows will present one article each. Two of these articles will be selected by the fellows from recent literature. The third will be selected from a list of landmark studies that have greatly affected the practice of critical care medicine. In addition to the presentation and an open discussion of the articles, the fellows will also discuss a statistical concept relevant to the chosen article. On a quarterly basis, instead of the standard format, a Pro-Con debate is presented. For this presentation, two fellows will pick a controversial topic related to critical care and present an evidence-based pro-con debate.
Morbidity and Mortality Conference
Once a month a divisional Morbidity and Mortality Conference is held in which three fellows present one case each to the other fellows and faculty with open discussion following the presentations. Approximately every two months, the critical care fellows presents their cases at the Department of Anesthesia’s departmental Morbidity and Mortality Conference, which is held on Wednesdays from 5:00-6:00 PM.
Critical Care Reading Program
A critical care reading program is available to guide fellows self-study. Each week, one chapter from a leading critical care text and 2 influential journal articles are assigned, and fellows meet with faculty every 2 weeks to discuss. This program effectively covers the breadth of critical care over the one-year fellowship period.
Clinical Education or Rotations
Core Intensive Care Unit Rotations
Nine months of the year-long fellowship are spent in the Surgical and Neurosciences Intensive Care Unit (SNICU) and Cardiovascular Intensive Care Unit (CVICU). The SNICU has four bays with a total of 30 beds and the CVICU (which is a mixed medical and surgical unit) will usually have 6-8 covered beds, depending on surgical census. Four teams cover the SNICU/CVICU (three based in the SNICU, one based in the CVICU). Fellows will rotate on an equal basis among the four teams, generally spending 2-4 weeks at a time with each team.
Elective Rotations
Up to three months may be spent in elective rotations relevant to critical care medicine. The two most popular electives are Echocardiography and Bronchoscopy. Other possible electives include, but are not limited to, Infectious Disease, Neurology, Nephrology, Medical Intensive Care, Pediatric Intensive Care, OR Anesthesia, Burn Surgery, and Research. Novel electives based on a fellow’s particular interests can be arranged with prior notification and approval. Electives are generally two or four weeks in length, depending on the rotation sponsor’s and fellow’s preferences.
Rotation Goals and Objectives
Goals and objectives are established for each rotation and can be reviewed here (note: UIowa/Internal access only)
Call Schedule
Call responsibilities are shared equally amongst all critical care fellows.
On weekdays (Monday through Friday), fellows take 24 hour, in-house call, with one fellow being on call each night.
On weekends (Saturday and Sunday), one fellow will cover both days (48 hours) on home call.
FAQ
How are the applicants chosen for interviews?
Applications are reviewed by a group of faculty. Based on the strength of the candidate and their application materials, an interview is offered.
Can you describe a typical clinic day for your fellows?
Fellows generally show up at around 7:00am. Morning rounds start at 7:30 and are most often done by 9:30-10:00. Fellow lectures, journal clubs, morbidity and mortality conferences, etc. are from 10:00-11:00 several days per week. Afternoon/checkout rounds occur at 2:00pm and generally last one hour. After checkout rounds, the non-call fellows make sure any outstanding issues are taken care of and generally leave by 5:00pm.
Do you have an electronic record?
Yes, since November 2010 the University uses Epic for medical records, including documentation and orders.
Do fellows have an educational fund?
Yes. Fellows are allotted a fund of $2,400 to provide support for specific needs during the course of their training, including attendance at one national meeting (attendance at the Society of Critical Care Medicine’s annual meeting is highly encouraged).
What are your average duty hours?
Fellows average less than 60 hrs per week. Duty hours are tracked by MedHub.
Can you give me an overview of your clinical activities?
The fellowship is based in the Surgical and Neurosciences Intensive Care Unit (SNICU) and the Cardiovascular Intensive Care Unit (CVICU). Fellows actively participate in the care of all patients in these units and are exposed to a broad and comprehensive patient base encompassing all aspects of critical care medicine. Experiences include, but are not limited to, complicated post-operative patients (solid organ transplant, heart and lung transplant, ventricular assist devices and total artificial heart, major vascular, etc.), neurological disease (stroke, intracranial bleed, neoplasm), trauma, respiratory failure/ARDS, cardiac failure and ischemia, liver and kidney dysfunction, and sepsis. The critical care service is responsible for all ventilator management, invasive monitoring, and coordination of care among the participating services. There is a particular emphasis on non-invasive cardiac output monitoring and procedural and diagnostic ultrasound.
How is fellow performance evaluated?
Faculty evaluate fellows quarterly using MedHub and the director meets semiannually, and as needed, with each fellow to review these evaluations and develop corrective strategies if indicated. The evaluations are based on the six ACGME core competencies. Nursing and other support staff also evaluate the fellows quarterly. These evaluations are also reviewed with the fellow during their semiannual meeting with the director.
Do fellows educate other trainees?
Yes. Residents of all training levels from multiple services rotate through the SNICU. In addition, the SNICU rotation is a popular elective among third and fourth year medical students. Fellows are encouraged to be active in both the clinical/bedside education of these learners as well as participating in didactic lectures to residents and medical students.
Emergency Medicine Critical Care (EMCC) Track
Welcome to the University of Iowa Emergency Medicine Critical Care Multidisciplinary Track of the Anesthesia Critical Care Fellowship. Critical care is one of the fastest growing subspecialties in emergency medicine, and the University of Iowa is offering a 2-year comprehensive, interdisciplinary fellowship to train the next generation of emergency medicine critical care leaders. Our program is based in the Department of Anesthesia with clinical rotations throughout the 811-bed University of Iowa Hospitals & Clinics, and with cooperation from the Department of Emergency Medicine, the Department of Surgery, and the Division of Pulmonary, Critical Care, and Occupational Medicine. Fellows will be training alongside fellows in other critical care fellowship programs, offering a rich environment for interdisciplinary training. Graduates will be eligible for certification through the American Board of Emergency Medicine Anesthesia Critical Care Medicine Pathway.
The Emergency Medicine Critical Care Track is a distinct track of the Anesthesia Critical Care Fellowship that prepares emergency medicine graduates for a broad-based multispecialty critical care practice.
Our fundamental philosophy is:
- To train excellent critical care clinicians with a broad multi-specialty critical care experience to manage diverse critical care patient populations in both academic and community settings,
- To advance the specialty of emergency medicine-critical care through scientific discovery, medical education, and quality improvement through ICU administration, and
- To develop leaders in emergency medicine to advocate for continuity of critical care from the prehospital environment through the emergency department, the intensive care unit, and recovery from critical illness.
With four pathways to board-certification now available to emergency physicians, we are excited to be on the forefront of training emergency medicine intensivists. We are looking for applicants who want to shape this movement through teaching, research, practice, and advocacy. You are joining a select group of emergency medicine intensivists, and we are excited that you are interested in joining us.
Quick Facts
- Multispecialty training in surgical, medical and subspecialty critical care
- 811-bed hospital with 103 adult critical care beds
- Rotations in 4 adult critical care units
- The University of Iowa Hospitals & Clinics Emergency Treatment Center is a new facility (opened in 2009) that sees approximately 60,000 patients annually
- ACGME-accredited critical care fellowships in anesthesia critical care, surgical critical care, pulmonary and medical critical care
- ACGME-accredited emergency medicine residency with 27 current residents
- Located in a progressive Midwestern university community with excellent schools, recreation, and ranked as one of the top 5 Most Livable Cities in America (Livability 2018)
Program Certification
The University of Iowa has had an Anesthesia Critical Care Fellowship continuously accredited since 1994. The American Board of Anesthesia has approved the emergency medicine track curriculum, and graduates will be eligible for Anesthesiology Critical Care Medicine board certification through the American Board of Emergency Medicine.
EMCC Applicant Information
How to Apply
The University of Iowa Anesthesia Critical Care Fellowship utilizes the Central Application Service, administered by San Francisco Match.
Candidates must apply to our fellowship by going to SF Match and using this service to submit an application. Their website gives instructions on registering for the match process, as well as how to submit the application and supplemental documents.
For the Letters of Recommendation, one should be from your residency program director and at least one from a critical care physician with whom you have worked.
Successful applicants will be invited for an on-site interview.
Additional information about this process can be found on the Society of Critical Care Anesthesiology website.
Board Certification
Graduates of the fellowship program are eligible for board certification through the American Board of Emergency Medicine in Anesthesiology Critical Care Medicine. This curriculum has been approved by the American Board of Anesthesiology and the program is a fully accredited fellowship.
Eligibility Criteria
Applicants must be graduates of a 3-year or 4-year ACGME-accredited emergency medicine residency program and be either board-certified or board-eligible by the American Board of Emergency Medicine (ABEM) or the American Osteopathic Board of Emergency Medicine (AOBEM). Board-certified applicants must meet the requirements of their applicable Maintenance of Certification program and have a valid unrestricted medical license. All applicants must complete 4 months of critical care as part of their residency curriculum.
EMCC FAQs
Will I be eligible for board certification in critical care after completion of this fellowship?
Yes. You will be eligible for Anesthesiology Critical Care board certification through the American Board of Emergency Medicine on successful completion of this fellowship. This curriculum has been approved by the American Board of Anesthesiology and the program is a fully accredited fellowship.
Will I be working in both medical and surgical ICUs during this fellowship?
Yes. The primary focus of this fellowship is on producing excellent clinical intensivists. The curriculum was designed such that approximately 1/3 of your critical care months will be medical critical care, 1/3 will be surgical critical care, and 1/3 will be specialty critical care (neurosciences, cardiac, etc.). Because some of these patient populations co-exist in the same critical care units, your allocation between ICUs may seem asymmetric, but we strive to keep this balance in your unit assignments and didactics to optimize the breadth of your critical care experience.
I am very interested in research. Can I modify my second year to incorporate more research time?
We have opportunities for involvement in both clinical and basic science research during your fellowship. Because of the program requirements for ACCM programs, no more than 2 months of your fellowship can be devoted to research activities, but nonclinical time is available throughout your fellowship to pursue research activities. The University of Iowa is a “very high research activity” institution according to the Carnegie Foundation, and multiple research mentors are available for you to pursue your research interests.
Will I be working shifts in the emergency department as part of my fellowship?
You will not be working in the emergency department at the University of Iowa, but there are opportunities for moonlighting at other local hospitals. Our philosophy is that your first priority is to learn critical care medicine, so we require that moonlighting not interfere with your primary responsibilities as a fellow.
What other critical care fellowships are offered at the University of Iowa?
The University of Iowa has well respected ACGME accredited fellowships in:
EMCC Educational Curriculum

Overview
The Emergency Medicine Critical Care Fellowship offers a range of clinical, didactic, and research training opportunities.
Clinical critical care training is based in three intensive care units at the University of Iowa: the 36-bed Surgical and Neurosciences Intensive Care Unit, the 26-bed Medical Intensive Care Unit, and the 24-bed Cardiovascular Intensive Care Unit. Rotations are also available in other clinical units and services at the University of Iowa.
- Surgical and Neurosciences Intensive Care Unit (SNICU) – The 36-bed SNICU is the largest intensive care unit in Iowa. As an American College of Surgeons-designated Level 1 Trauma Center and a Joint Commission-accredited Comprehensive Stroke Center, the SNICU cares for patients with critical traumatic injuries, general surgery, neurosurgery, otolaryngology, transplant, neurology, and stroke patients. Residents from emergency medicine, anesthesia, general surgery, neurosurgery, neurology, family medicine, otolaryngology, orthopedic surgery, and oral surgery rotate through the SNICU.
- Medical Intensive Care Unit (MICU) – The 26-bed MICU is the largest medical ICU in Iowa, and it provides comprehensive medical care for critically ill medical patients. Emergency Medicine and Internal Medicine residents rotate through the MICU, and this unit manages most V-V ECMO for severe respiratory failure at the University of Iowa.
- Cardiovascular ICU – The 24-bed CVICU was opened in April 2014, and provides care for patients with acute coronary syndrome, heart failure, and surgical patients after cardiac, thoracic, and vascular surgery procedures. Two physician teams provide comprehensive critical care for patients with both medical and surgical emergencies. As the only Joint Commission-certified Ventricular Assist Device Program in Iowa, patients are treated with a variety of mechanical cardiovascular support devices.
Curriculum
The comprehensive 24-month curriculum has been designed to provide fellows the most broad exposure to multidisciplinary critical care. The program was approved by the American Board of Anesthesiology to qualify graduates for board certification in the Anesthesiology Critical Care pathway through the American Board of Emergency Medicine.
The curriculum is arranged in 13 4-week blocks each year.
| Year 1 (13 blocks) | Number of Weeks |
| Surgical Critical Care (within Surgical and Neuro ICU) | 12 weeks |
| Cardiothoracic Critical Care (Surgical) | 4 weeks |
| Neurological Critical Care (within Surgical and Neuro ICU) | 8 weeks |
| Medical Critical Care | 8 weeks |
| Surgical Selective | 8 weeks |
| Cardiothoracic Surgery and Cardiac Anesthesiology | 3 weeks |
| Fiberoptic Bronchoscopy and Chest Procedures, ICU Nutrition | 3 weeks |
| Clinical Electives/Research | 3 weeks |
| Vacation | 3 weeks |
| Year 2 (13 blocks) | |
| Surgical Critical Care (within Surgical and Neuro ICU) | 12 weeks |
| Cardiothoracic Critical Care (Surgical) | 8 weeks |
| Neurological Critical Care (within Surgical and Neuro ICU) | 4 weeks |
| Medical Critical Care | 8 weeks |
| Cardiac Critical Care | 3 weeks |
| Critical Care Selective (SNICU, MICU, PICU) | 4 weeks |
| Clinical Electives/Research | 10 weeks |
| Vacation | 3 weeks |
Available Clinical Electives (not exclusive):
- Advanced echocardiography (including transthoracic echocardiography)
- Advanced inpatient trauma care
- Burn Surgery
- Extracorporeal life support (ECMO)
- Nutrition
- Pediatric critical care
- Pharmcology (with clinical pharmacists)
- Renal and hemodialysis medicine
- Rehabilitation medicine
- Transplant medicine (solid organ/bone marrow)
- Research
- Other rotations at discretion of program director
- Optional longitudinal electives
Fellows will participate in clinical and call activities in accordance with the ICU to which they are assigned. Fellows will have a co-supervisory role for residents and medical students assigned to ICUs in which they are rotating, and are expected to participate in resident and medical student teaching activities.
Fellows will be evaluated monthly by their supervising faculty using an online evaluation tool, and biannual summative evaluations with the program director will review ongoing progress toward preparation for independent critical care practice.
Education and Conferences
A wide variety of critical care didactic curricula are available for critical care trainees. Both medical and surgical ICUs have weekly didactic programs, and fellows are encouraged to participate in the didactic training of the unit where they are working. Didactic training covers the breadth of medical and surgical critical illness, journal clubs and evidence based-medicine, and case conferences and presentations. Fellows participate in a reading program with asynchronous resources available to supplement their critical care didactic program. Fellows are required to present cases and lectures in conferences.
Fellows are required to participate in two non-clinical projects during their fellowship: a scholarly activity and a quality improvement project. The academic project could be comprised of original research, writing, review articles or book chapters, or another contribution to the development or dissemination of critical care knowledge. The quality improvement initiative will take the trainee through the plan-do-study-act methodology of quality improvement to learn the methods of continuous improvement in large complex organizations.
Fellows have $2400/year in academic funds that can be used for conference travel, professional memberships, books, and other educational resources to supplement the educational program.
Teaching
One important aspect of development as a clinician-educator is learning how to teach effectively. Intensivists in academic practice clearly have a teaching component of their career, but community intensivists also fill an important niche in teaching nursing staff, allied health professionals, and colleagues. Fellows will refine their teaching activities through resident and medical student clinical teaching. In addition, the College of Medicine’s Office for Consultation and Research in Medical Education and the Fellows as Clinician Educators programs both support advanced training in clinical teaching.
Research
Faculty members at the University of Iowa are engaged in clinical, basic science, health services, and educational research. The Institute for Clinical and Translational Science is a resource for faculty and fellows pursuing research interests. A variety of ongoing projects are available for fellows to learn research methods, or fellows can create their own research project. Regular clinical release time is available for fellows to pursue academic activities, including research, writing, curriculum development, and other academic activities upon approval by the program director.
EMCC Fellowship Longitudinal Electives
The critical care fellowship has established a series of optional longitudinal electives as part of the curriculum. While these are not required, these curriculum tracks offer the fellow more in-depth experience for developing additional qualification, certification, or competence during the critical care fellowship. These longitudinal electives will consist of dedicated month(s) of elective, in addition to a sustained exposure to the topic of interest during a 6-month period of the fellowship. The currently available tracks are listed below:
Extracorporeal life support
This elective consists of a 1-week course in extracorporeal life support management, followed by 2 weeks of dedicated time learning from the ECMO physicians and specialists. Following the dedicated 3-week elective, the fellow will take call with the ECMO team and round on ECMO patients in the cardiovascular ICU (venoarterial ECMO) and the medical ICU (venovenous ECMO).
Transthoracic echocardiography
This elective consists of an introduction to cardiac echo, followed by 2 months of 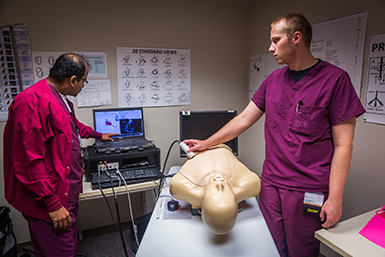 dedicated rotations in the echocardiography laboratory. During these rotations, fellows will be performing formal echocardiograms (in both critically ill and non-critically ill patients and interpreting echocardiograms with cardiologists specializing in echo interpretation. After the elective time, fellows will spend some afternoons on other rotations performing and interpreting echocardiograms, with the goal of 300 echo interpretations and 150 supervised echocardiograms. At the conclusion of this 6-month experience, the fellow will have sufficient training and experience to sit for the American Board of Echocardiography Transthoracic Echocardiography Board exam, and would qualify for Testamur status on successfully passing the examination.
dedicated rotations in the echocardiography laboratory. During these rotations, fellows will be performing formal echocardiograms (in both critically ill and non-critically ill patients and interpreting echocardiograms with cardiologists specializing in echo interpretation. After the elective time, fellows will spend some afternoons on other rotations performing and interpreting echocardiograms, with the goal of 300 echo interpretations and 150 supervised echocardiograms. At the conclusion of this 6-month experience, the fellow will have sufficient training and experience to sit for the American Board of Echocardiography Transthoracic Echocardiography Board exam, and would qualify for Testamur status on successfully passing the examination.
Percutaneous dilatational tracheostomy
This elective consists of a dedicated 2-day course in percutaneous tracheostomy placement, followed by structured meetings with the acute care surgeons who perform bedside percutaneous tracheostomy at the University of Iowa. After the didactic portion of this rotation, fellows will observe 5 tracheostomy procedures, then will perform 15 percutaneous tracheostomy procedures with graded levels of responsibility (consistent with training requirements recommended by American College of Chest Physicians and American Thoracic Society).
Inter-hospital transfer
This elective starts with a one-month EMS experience incorporating air transport,  ground transport, EMS education, and EMS administration components. Fellows will fly on AirCare, the University of Iowa helicopter aeromedical transport service. They will provide direct clinical care during their shifts, and they will have a didactic and reading program focused on the administration of EMS services, especially for critically ill patients undergoing interfacility transfer. Over the remainder of a one-year experience, they will be scheduled for AirCare shifts and providing continuing prehospital provider education as well.
ground transport, EMS education, and EMS administration components. Fellows will fly on AirCare, the University of Iowa helicopter aeromedical transport service. They will provide direct clinical care during their shifts, and they will have a didactic and reading program focused on the administration of EMS services, especially for critically ill patients undergoing interfacility transfer. Over the remainder of a one-year experience, they will be scheduled for AirCare shifts and providing continuing prehospital provider education as well.
EMCC Fellows and Graduates
Current Fellows, Emergency Medicine Track (2023-2024)

Jordan Miller, DO, Summa Health System
(Second Year)

Joseph Crum, DO, Ohio Health
(First Year)

Steven Ilko, MD, Spectrum Health
(First Year)

Marc Toofan, MD, Scott and White
(First Year)
GRADUATES
Emergency Medicine track (2021-2023)

Erin Evans, MD, University of Iowa

Jenna Lizzo, MD, University of Illinois

Rachel Posey, DO, John Peter Smith Health Network
Emergency Medicine track (2020-2022)

Erik Campbell, MD, University of Tennessee
Emergency Medicine track (2019-2021)

Alysa Davis, DO, University of Iowa

Benjamin Rezny, DO, MA, University of Tennessee Health Science Center
Emergency Medicine track (2018-2020)

Brad Johnson, MD, Henry Ford Hospital

Aaron Tyagi, MD, Michigan State University
Emergency Medicine track (2015-2017)

Robert Plambeck, MD, Eastern Virginia Medical Center

Ryan Dick-Perez, DO, Summa Health Center
Contact Us

Archit Sharma, MD MBA
Fellowship Director
Department of Anesthesia
200 Hawkins Drive, 6512 JCP
Iowa City, IA 52242-1079
Phone: 1-319-384-7911
Fax: 319-356-2940
archit-sharma@uiowa.edu

Nick Mohr, MD
Assistant Fellowship Director, EMCC Track
Departments of Emergency Medicine and Anesthesia
200 Hawkins Drive, 1008 RCP
Iowa City, IA 52242-1009
Phone: 1-319-384-6511
nicholas-mohr@uiowa.edu

Tammi Steffen, BS
Critical Care Fellowship Coordinator
Department of Anesthesia
University of Iowa Hospitals & Clinics
200 Hawkins Drive, 6546 JCP
Iowa City, Iowa 52242-1079
Phone: 1-319-356-7205
tammi-steffen@uiowa.edu
Program Accreditation & Board Certification
Program Accreditation
The anesthesiology critical care medicine fellowship at the University of Iowa Hospitals & Clinics is a one-year Accreditation Council for Graduate Medical Education accredited program. The program is approved for 4 total fellow positions.
Information specific to program requirements for an anesthesiology critical care medicine training program and milestones for fellow performance may be found at the ACGME’s Anesthesiology Review Committee (RC).
Board Certification
The ABA-American Board of Anesthesiology-certifies physicians in critical care medicine by administering the Critical Care Medicine examination. Our fellowship program expects fellows to become certified in Critical Care Medicine.
The critical care medicine physician is a specialist whose knowledge is of necessity broad, involving all aspects of management of the critically ill patient, and whose primary base of operation is the intensive care unit (ICU). This physician has completed training in a primary specialty and has received additional training in critical care medicine aspects of many disciplines. This background enables the physician to work in concert with the various specialists on the patient care team in the ICU; to utilize recognized techniques for vital support; to teach other physicians, nurses and health professionals the practice of intensive care; and to foster research.
Subspecialty certification is detailed in the ABA's BOI (Booklet of Information).
How to Apply
The University of Iowa Anesthesia Critical Care Fellowship utilizes the Central Application Service, administered by SF Match. Candidates must apply to our fellowship by going to SF Match and using this service to submit an application. Their website gives instructions on registering for the match process, as well as how to submit the application and supplemental documents.
Additional information about this process can be found on the Society of Critical Care Anesthesiology website.
Applications are reviewed and suitable candidates will be invited for an interview.
Deadlines
The application and interview season runs from November to February. Applicants should apply in their second to last year of residency (for Anesthesia residents this would be the CA-2 year) as the match occurs approximately 14 months prior to the start of the fellowship year. For instance, fellows interviewing in the 2023-2024 academic year will match in May 2024and will begin their fellowship in July 2025.
While there is no hard deadline for the submission of applications, applicants should be mindful that rank lists are due late May and thus, applications must be submitted early enough to allow for scheduling and completion of interviews prior to this date.
Fellow Eligibility
Eligibility criteria for applicants:
1. Graduate from one of the following:
- United States or Canadian medical school accredited by the Liaison Committee on Medical Education (LCME)
- United States college of osteopathic medicine accredited by the American Osteopathic Association (AOA)
- Medical school outside the United States or Canada with:
- A valid certificate from the Educational Commission for Foreign Medical Graduates (ECFMG) and have a passing score for Step 1 and Step 2 of the USMLE
- Be a U.S. citizen, a legal permanent resident, or hold a visa which provides eligibility to work in the U.S. Typical visas are J-1 (requires Steps 1 and 2 of USMLE and ECFMG certification) and H1-B (requires departmental approval, and Steps 1, 2 and 3 of USMLE, and an Iowa medical license)
2. Meet Iowa Board of Medicine licensure requirements.
3. All applicants must also meet program eligibility requirements as defined by the ACGME’s respective RRC.
Contact our Fellowship Coordinator if you have any eligibility questions.
The Department of Anesthesia at Roy J. and Lucille A. Carver College of Medicine and UI Health Care shares the University of Iowa’s commitment to equal access and, consistent with its academic mission and standards, strives to achieve excellence through the advancement of diversity, equity, and inclusion. In the Department of Anesthesia, we are mindful of all aspects of human difference and define diversity in the broadest sense to mean inclusion of all persons. This means we do a holistic review of applications, with particular interest in recruiting applicants who have shown grit and resilience in their path to medicine, as well as potential to lead anesthesiology in the future.
Fellowship Interviews
The Interview
To minimize health risks associated with travel during the COVID-19 pandemic, and in compliance with institutional, state, and national recommendations, we will conduct all interviews will be conducted online only. We will not offer any in-person interviews or site visits during this cycle. The online-only interview requirement applies to all candidates, internal or external, so that we may provide an equitable experience to all applicants.
We plan to interview candidates beginning in December and ending in February. Match Day for the Critical Care Fellowship is generally in May for the following July 1 start.
Invitations to interview
Interview invitations from our program will be extended via SF Match. You will be able to see available times and dates and self-schedule your interview.
What should I expect on the interview day?
We plan to conduct interviews on the Zoom platform. The interview day includes an overview of the program, a virtual tour, and interviews with the program director, current fellows, and Anesthesia Critical Care faculty.
Our People
Program Faculty
Archit Sharma, MBBS, Program Director, Critical Care Medicine Fellowship
Lovkesh Arora, MBBS, MD
James Blum, MD
Anita Chazhikattu, MBBS Associate Program Director, Critical Care Medicine Fellowship
Brent Hadder, MD
David Kaczka, MD, PhD
Nick Mohr, MD, MS Program Director, Emergency Medicine Critical Care Fellowship Track
Mark Pedersen, MPH, MD
Jonathan Simmons, DO, MS Associate Program Director, Critical Care Medicine Fellowship
Shawn Simmons, MD
Current and Graduate Fellows
Current Fellows (2023-2024)
Emergency Medicine Track, First Year
Joseph Crum, DO
Steven Ilko, MD
Marc Toofan, MD
Emergency Medicine Track, Second Year
Jordan Miller, DO
Graduates

Erin Evans, MD (2021-2023)

Jenna Lizzo, MD (2021-2023)

Rachel Posey, DO (2021-2023)
Erik Campbell, MD (2020-2022)

Alysa Davis, DO (2019-2021)

Benjamin Rezny, DO (2019-2021)
Brad Johnson, MD (2018-2020)

Aaron Tyagi, MD (2018-2020)
Graduates (2018-2019)
- Alex Suginaka, DO, Critical Care Medicine Fellow
- Bharathram Vasudevan, MD, Critical Care Medicine Fellow
Graduates (2017-2018)
- Michael Hicks, DO, University of Iowa
- Luke Linz, DO, University of Iowa
- Anna Riessen, MD, University of Iowa
- Adrienne Samar, MD, University of Iowa
Graduates (2016-2017)
- Anita Chazhikattu, MBBS, University of Iowa
- Alexandra Chludzinski, MD, University of Iowa
- Sara Herrera, MD (Surgery), St. John Hospital, Detroit
- Jennifer Shanklin, MD (Surgery), University of Iowa
Graduates (2015-2017)
- Emergency Medicine Track
- Ryan Dick-Perez, DO, Summa Akron City Hospital
- Robert Plambeck, MD, Eastern Virginia Medical School

